On September 18, the Center for Medicare and Medicaid Innovation (CMMI) announced its new Radiation Oncology (RO) Model, the first mandatory bundled payment program since the Comprehensive Care for Joint Replacement Program (CJR) started in 2016. The RO Model is slated to start January 1, 2021, and is expected to continue for five years.
According to CMMI, “The RO Model tests whether bundled, prospective, site neutral, modality agnostic, episode-based payments to physician group practices (PGPs), hospital outpatient departments (HOPD), and freestanding radiation therapy centers for radiotherapy (RT) episodes of care reduces [sic] Medicare expenditures while preserving or enhancing the quality of care for Medicare beneficiaries.”
The details regarding the RO Model are contained in a nearly 1,000-page final rule, which also covers the new ESRD Treatment Options Model. Many of those pages are devoted to explaining CMMI’s methodology for selecting those providers that will be required to participate in the RO Model.
As with CJR, CMMI is making participation in the RO Model mandatory, rather than voluntary, to eliminate the impact of self-selection on the model’s outcomes. To ensure confidence in those results, CMMI randomly selected a sufficient number of RT providers and suppliers to account for 30% of all RT episodes nationwide.
For CJR, CMMI identified the hospitals subject to mandatory bundled payments for certain joint replacement surgeries by metropolitan statistical areas (MSAs). All hospitals physically located in one of the selected MSAs were included in the program unless excluded for a specified reason.
By contrast, CMMI is using core-based statistical areas, or CBSAs, to identify RO Model participants. CMMI has linked RT providers and suppliers to a CBSA by using the five-digit ZIP Code of the location where RT services are furnished. As with CJR, all providers furnishing RT services in the selected ZIP Codes will be included as model participants unless excluded for one of the reasons specified in the final rule.
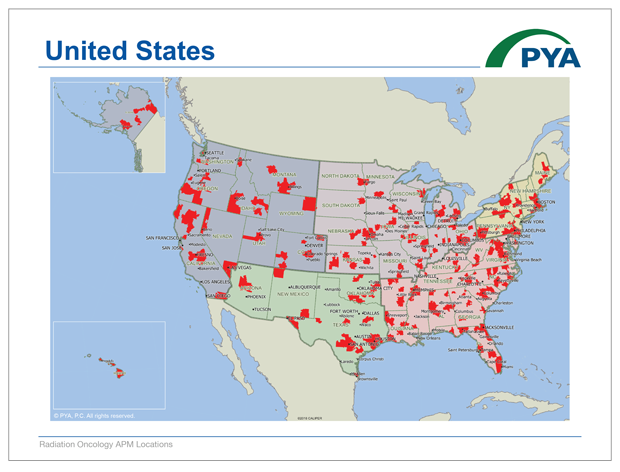
To identify the selected RO Model participants, CMMI released an excel spreadsheet listing 9,000 ZIP Codes—with no other identifying information (e.g., name, city, state). PYA has converted those ZIP Codes into a map to illustrate the reach of the RO Model.
Click Below to View the PDF Map or View the Google Map Below (load times vary):
In place of fee-for-service reimbursement, RO Model participants will receive episodic payments split into a professional component (PC) payment (which represents payment for those RT services furnished by a physician) and a technical component (TC) payment (which represents payment equipment, supplies, personnel, and costs related to RT services). Half of the episode payment amount will be paid when the RO episode is initiated, and the balance will be paid at the conclusion of the 90-day episode.
CMMI will determine RO participant-specific episodic payment amounts for 16 common cancer types based on proposed national base rates, trend factors, and adjustments for each participant’s case-mix, historical experience, and geographic location. CMMI then will apply a 3.75% discount factor to the PC payment and a 4.75% discount to the TC payment. Finally, CMMI will withhold 1% from all payment amounts for incorrect payments, 2% from PC payments for quality, and, starting in 2023, 1% from TC payments for patient experience. RO participants can earn back all or some of these withholdings based on actual performance.
If you find your organization in one of these ZIP Codes, contact a PYA executive below at (865) 673-0844 to discuss what you should be doing now to prepare for the scheduled January 1, 2021, start date for the RO Model.
UPDATE: October 30, 2020:
CMS announced it intends to delay the RO Model start date to July 1, 2021. However, selected RO Model participants should not delay preparing for this change. Read PYA’s updated insight, “CMS Delays Start Date of Radiation Oncology Mandatory Bundled Payment Program,” for the latest guidance.




